|
There are a number of reasons that adults—grown adults—avoid trips to the dentist.
According to the American Dental Association, over 17% of people admit they avoid going to the dentist due to anxiety. And this “demotivator” is right behind the very real inability to pay for dental services that leaves millions of patients avoiding appointments each year. There are still others who have special needs or who are facing complex dental procedures, which result in fear or apprehension when faced with a visit to the dentist.
If you or a family member—even children--can identify with any of these issues, then it might be worthwhile to consider if sedation dentistry is right for you. Don’t let the word “sedation” cause more anxiety, though! This option is a safe and gentle for almost all ages. Keep reading as we break down the types of sedation available as well as the groups of patients who may be best served by sedation dentistry. What is sedation dentistry?
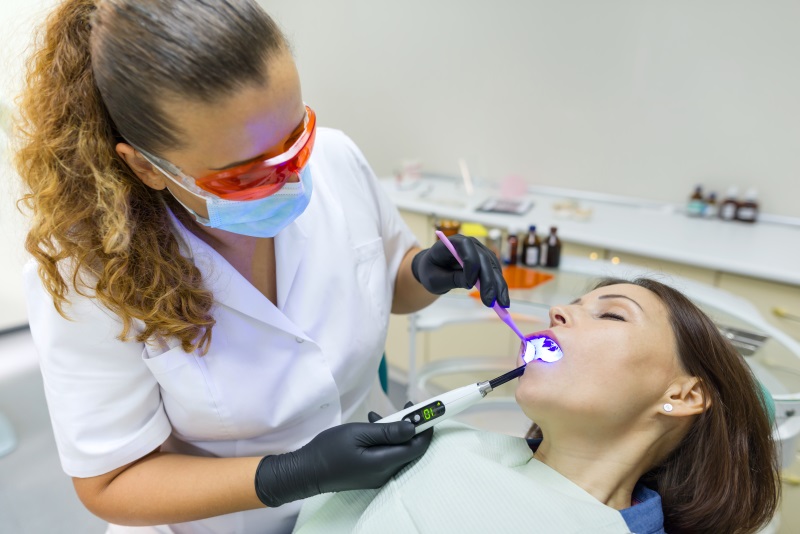
Sedation dentistry offers patients relief from anxiety and pain and ensures a pain–free procedure--many times without any memory of the appointment. While many complex procedures are performed with some form of anesthesia, it is possible for general cleaning to also take place under sedation for those patients who suffer from severe anxiety.
There are several levels of sedation we use, all depending on the complexity of the procedure. The American Dental Association, in conjunction with state guidelines, offers a set of best practices for the administration of local anesthesia, sedation, and general anesthesia. Your dentist will decide which level of sedation is best for you. Below is a breakdown of the varying types of anesthesia typically used:
Who’s eligible for sedation dentistry?
Anxious patients
As mentioned, dental anxiety is a highly present issue among adults. If you suffer from dental anxiety, but have trouble articulating your fears with your dentist, your provider might choose to utilize the Corah’s Dental Anxiety Scale. Developed in 1969, this four question survey allows patients to choose from five answers. Each answer corresponds with numerical score. The total score allows the dentist to determine how anxious you are about the appointment.
Another assessment tool is the Modified Dental Anxiety Scale. This survey consists of five questions, each with a five-category rating scale, ranging from “not anxious” to “extremely anxious.” One difference in this survey is that it has an extra item about the respondent’s anxiety to a local anesthetic injection as well as the dental procedure itself.
Based on the results of the survey, your dentist may recommend sedation as part of your treatment.
Special needs patients
The special needs population is diverse and has a wide range of dental needs. Due to this, the reasons for the use of sedation dentistry are equally varied. Not only does this influence the type of anesthesia used, it also makes an impact on how the anesthesia is introduced.
For instance, special needs patients may have physical limitations as well as intellectual disabilities, each of which are vital components that are taken into consideration. One common example of special needs dentistry is serving those with autism. Since the dentist’s office can present an array of sensory challenges such as new tastes, smells and textures, sedation can offer a calmer experience. If you or your child have special needs, have a conversation with your dentist ahead of time to discuss options to make the patient most comfortable.
Complex procedures
Finally, some dental procedures can take several hours to complete. Since many patients would prefer to be in the chair for the least amount of time possible, they choose to break these procedures into multiple visits. However, sedation density allows patients to calmly complete complex procedures in a single visit. For example, patients who need extensive rebuilding procedures or multiple cavities filled at one time may be good candidates for sedation dentistry.
Are there risks to sedation dentistry?
As with any procedure, it’s important to discuss with your dentist if you are a good candidate for sedation dentistry. For those with sleep apnea or adverse reactions to anesthesia, it’s important to discuss your medical history with your dentist prior to any procedure.
Finally, everyone reacts differently to the different medications used for sedation. This includes how much is needed for complete sedation as well as any adverse feelings upon “coming to.” If you are concerned about how you may react, make sure to ask your dentist prior to your appointment.
Sedation dentistry has the ability to transform the practice of dentistry for those that avoid it due to anxiety or fear of pain. If you are interested in what Dr. Ku’s office has to offer, give us a call today! The post Sedation Dentistry – Your Ultimate Guide appeared first on Fort Worth Dentist | 7th Street District | H. Peter Ku, D.D.S. PA. via Blogger Sedation Dentistry – Your Ultimate Guide
0 Comments
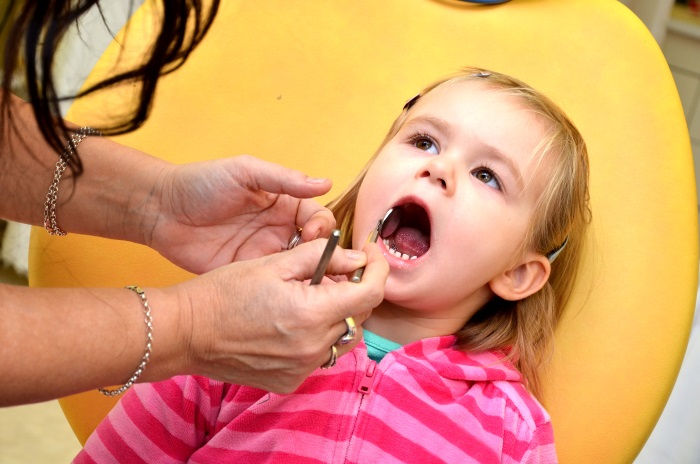
How happy do you feel when you see your child completing milestones? The first step, the first word, and the first smile. These are all wonderful experiences that a parent will never forget. We’re sure you felt a leap of joy when you saw your child had sprouted his or her first tooth, too. And that joy is natural because, at this stage, that will also mean your babe will soon be eating a more diverse diet, too. After celebrating this event, it’s also time to think about another “first” for your child—his or her first visit to the dentist. Starting dental visits at a young age can greatly increase the odds that your child will maintain good oral health and a sparkling white smile through life. But how do you get your child prepared for the chair? Are you concerned the experience will be intimidating? Let’s jump in and see how you can quickly and simply get your child read! When should a child visit the dentist for the first time? In general, it’s recommended that children should have their first dental visits no more than six months after the appearance of their first tooth. Starting dental visits at such a young age can play an important role in the oral health of your child later in life. To begin with, baby teeth may not be permanent, but they can cause issues in speaking and chewing if they are not healthy. What’s more, tooth decay can occur as soon as your child’s first tooth pops, and having tooth decay on baby teeth can further increase the risk of having tooth decay in permanent teeth. And, perhaps the most important reason yet, starting dental visits at a young age can help build the habit of proper dental care and grow familiarity with dental procedures so that these don’t cause anxiety in the future. Building these routines at such a young age can greatly increase the odds that your kids will keep those healthy habits throughout life. How to prepare your child for the first dentist visit The first dental visit for your child can end up being frightening—for your child and for you—if he or she isn’t prepared. But these simple tips can help get everyone on board for a stress-free dental visit! Tip #1: Practice at home It’s very important for your child to get accustomed to having hands and fingers in and around the mouth before visiting the dentist for the first time. What’s a hygienic and safe way to go about this? Try Running a soft, wet washcloth or a toothbrush specially designed for infants over the gums and teeth. This both cleans your child’s teeth and gets him or her accustomed to having hands and dental tools in the mouth. Songs and games can reinforce this routine. Tip #2: Begin teaching your child about teeth Children love exploring and learning new things! Teaching your child about his or her teeth and mouth will not just be a way to get interested in oral health, but will also make the first dental appointment easier. Since we’re talking about starting these practices at a very young age, simply teaching your child to identify where everything is in its mouth is enough for now. Songs, games, giving names to teeth can help here as well! Tip #3: Explain what to expect at the dentist’s office to your child Your child’s first dental visit will not involve any pain. The dentist will devote time to gently examine your child’s teeth--and maybe clean them if necessary. At Dr. Ku’s office, we make the visit a fun experience in order to create a positive association with dental visits. In addition, games like using a stuffed animal as a “dentist” in play or teaching your child how to be the dentist by allowing him or her to “examine” your teeth will definitely be fun and help your child become familiar with the process.
Your child’s first dental appointment can very easily become a fun experience if you practice beforehand with fun and games! Follow the list above, and you will experience a tear-free first visit. The post How to Prepare Your Child for the First Trip to the Dentist appeared first on Fort Worth Dentist | 7th Street District | H. Peter Ku, D.D.S. PA. via Blogger How to Prepare Your Child for the First Trip to the Dentist We’ve all experienced toothaches. They can be mild or severe, and can be caused by a variety of factors, with a small portion of them being critical.
If you aren’t suffering from a serious oral or dental issue, most of these toothaches will go away in less than a day with pain killers and some home remedies like saltwater rinses, compresses and clove oil. However, sometimes the problem isn’t quite so simple. Imagine having a severe, persistent toothache that radiates down your neck, ears, and jawbone. You take painkillers and use every home remedy available in your arsenal, but the pain still doesn’t go away. In addition, you have a fever and swollen lymph nodes in your neck, and you experience sensitivity to chewing, cold, and hot foods, and even experience swallowing or breathing difficulties.
If this is ever the case, you might be suffering from a periapical abscess. A periapical abscess is an infection on one of your teeth and it is considered a critical oral health issue. A periapical abscess can cause you to lose the infected tooth and, if not treated properly, it can cause serious or even life-threatening complications.
In this article, we’re going to break down what a periapical abscess is, what causes it, what treatment methods are available, and some pain–relieving home treatments to try while you wait to see your dentist. In any case, make sure to see your dentist as soon as possible if you suspect you’re suffering from an abscess.
Fast facts on dental abscesses
A dental or tooth abscess is a pus pocket associated with a specific, damaged tooth. It can happen to patients of any age group and will not heal on its own. There are four types of abscesses that can occur in different regions of the tooth:
Every type of abscess has its own level of severity and set of symptoms. In this article, we’re going to focus on the periapical abscess.
Causes of a periapical abscess on a tooth
In a glance, a periapical abscess can happen when any bacterial infection makes its way into the innermost part of a tooth, the dental pulp. The dental pulp is the heart of our tooth because it contains its blood vessels and nerves.
However, we all know how hard our teeth are. As a result, bacteria making their way into the heart of a tooth isn’t going to happen overnight. Let’s break down the processes that ultimately allows bacteria to enter deep inside our pearly whites, later leading to complications like periapical abscesses.
To begin with, bacteria are present everywhere around and inside us. In fact, a study has shown that there are ten times more bacteria than human cells in the body, with a staggering number of 39 trillion bacterial cells inhabiting every one of us! A relatively small number of this colony (about 6 billion) inhabit the mouth.
Factors like diet, poor oral hygiene and plaque, can enable some of these bacteria to release acids. These acids will attach to the tooth enamel (which is the protective shield of our teeth) and then starts dissolving it, resulting in the formation of tiny holes on the teeth. These tiny holes have a very famous name: tooth decay!
If a tooth is cracked or has these tiny holes due to tooth decay, more bacteria can enter through them, dissolve the soft tissue layer under the enamel, and eventually find their way into our tooth’s heart (the pulp). There, they infect and wreak havoc on the tooth’s blood vessels, nerves, and connective tissue, and can end up killing the tooth in time.
However, the infection doesn’t end there. If the abscess is not treated, chances are that the infection will eventually spread to other areas, too, including the jaw, neck, and head, causing all sorts of infections including sepsis, which is life-threatening.
Symptoms of a periapical abscess
The main symptom of a periapical tooth abscess is pain. The pain is usually severe, but sometimes it can be tolerable. Other symptoms that may reveal a periapical tooth abscess include:
Note: The sum of these symptoms all at once makes for a critical situation. If you experience difficulties in breathing or swelling, get care immediately. If your dentist isn’t available, go to an emergency room as soon as possible.
Treatment and tips to ease the symptoms
A periapical tooth abscess can’t be treated at home and won’t just “go away on its own.” You have to visit your dentist as soon as possible if you experience the symptoms mentioned above or have reason to believe you might have developed a periapical abscess or other serious oral infection.
Dental abscesses are generally treated by removing the source of the infection and draining away the pus. Depending on the severity of the infection, possible treatments may include:
While you are waiting to see your dentist, here are some home tips that can help ease the symptoms of an oral periapical abscess:
To recap, a periapical tooth abscess is a critical infection that cannot be treated on its own. The home tips listed above can help you while waiting to see your dentist and can help with the pain and other symptoms. However, the most important thing is to see a dentist as soon as possible. The post Periapical Abscess: What it is, what causes it and how it’s treated appeared first on Fort Worth Dentist | 7th Street District | H. Peter Ku, D.D.S. PA. via Blogger Periapical Abscess: What it is, what causes it and how it’s treated You’ve probably heard before that oral health is a window to your overall health. Your healthy teeth, gums and smile reveal not just what lifestyle choices you’re making right now, but also what could be going on in the rest of your body in other systems. And beyond being a window into other things going on, cavities, gum issues and plaque can also have direct consequences to your overall health.
As if that isn’t enough to take your oral health seriously, there’s also the fact that, if you don’t take care of your teeth, you might be up needing some complex dental procedures that you would rather not need. We make all work done at our office as comfortable as possible for patients, but there won’t ever be a line out the door of patients wanting to sign up for root canals.
Simple advice such as brushing and flossing your teeth daily can be taken for granted, because we all know how essential these are for a healthy mouth. But simple though it should be, data show that only 50% of Americans brush their teeth twice per day, one in three brushes their teeth just once per day, and there is even an 8.6% of Americans that brush only once every few days (Authority Dental). As a result, we can clearly see that, although information and advice about oral health is widespread, our oral health is often forgotten.
Before digging into Ancient Medicine Today’s home tips for gaining and maintaining a healthy mouth, let’s examine which factors can cause higher risk (and greater need for care) for some patients:
Although we can’t see, feel, or taste them, there are more that 700 bacterial species inhabiting our mouth at any given moment (NCBI). Many of these bacteria feed on the processed sugars we consume and produce the waste products that cause cavities and other diseases.
Apart from a proper diet, strong oral routines and doing what you can to quit smoking, let’s see what some of the other tips are that Ancient Medicine Today’s video has outlined in such fantastic detail. These are habits that you can apply in the comfort of your home, and which can help you maintain good oral health more easily and avoid future complications.
Massaging the gums and flossing
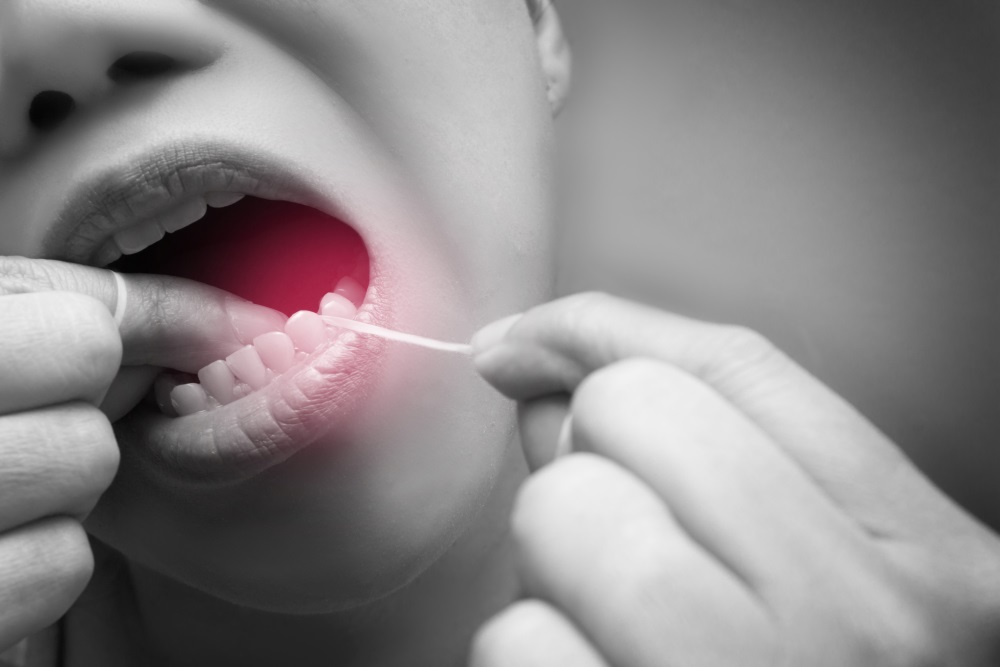
We try to mention flossing as often as we do teeth brushing, because they really do go hand-in-hand. You’ve heard it before, but try just for a moment to pay the same attention you would to a juicy new fact in a trivia game, because we want this information to stick. According to a study by lead author Duong T. Nguyen, only 30% of Americans floss daily, 37% floss less than daily, and over 32% never floss.
Flossing brings you all kind of oral health benefits, including keeping your smile bright, assisting in plaque removal, and preventing plaque build-up and the subsequent risk of gingivitis and gum disease. Flossing also reduces of bad breath and can make brushing your teeth more effective. So, the takeaway here is to always floss twice a day, right before you brush, to dislodge bits of food and clean the areas that your toothbrush can’t reach.
On the same subject of gums and gingivitis, massaging your gums can also bring benefits to your oral health. According to the Ancient Medicine Today video, massaging your gums can also help in plaque removal and the prevention of plaque build-up over time. They even recommend using a vibrating toothbrush to effectively massage your gums and ensure easier plaque removal and a sparkling white smile!
Clove oil and oil pulling
Clove oil is a worthy solution to mention for its natural properties that help solve toothaches. Clove oil contains eugenol, a chemical that has anesthetic and antibacterial properties. This natural solution has been used in dentistry since the 19th century (MTN).
When you are hit by a toothache, dip a clean cotton ball into the oil and apply it over the gums at the point of the pain. In addition, you can gargle clove oil diluted with water, just watch the video above to see how it’s done.
If you’re interested in similar options, other oils like coconut, sesame or olive oil are great ways to maintain oral health, too. According to many studies cited in the video, studies, these oils generate antioxidants which hinder bacteria growth by damaging the cell walls of microorganisms to kill them off. The microorganisms targeted include plaque-building bacteria responsible for dental cavities, gingivitis, periodontitis, and bad breath. These oils also help stop gum bleeding and can make your teeth whiter!
To apply these oils, simply swish a half or one teaspoon of oil in your mouth, and make sure you work it through all the areas between your teeth. After a few minutes, spit out and rinse your mouth well. This practice, called oil pulling, should be done once or twice a day, and it will naturally whiten your teeth and detox your mouth.
COQ10 and oral probiotics
Coenzyme Q10 or COQ10 can be found naturally in the body and is an important nutrient for gums that can have a positive impact in preventing gum disease and gum bleeding. COQ10 has anti-aging properties, too, and can improve exercise performance, heart health, and diabetes. A recommended dose of COQ10 is 90–200 mg per day.
Oral probiotics introduce friendly bacteria to your system. They include living microbes and foods containing living microbes, all of which beneficially influence your health when used on a daily basis or even as-needed (NCBI). Studies have shown that specific oral health probiotics can prevent all oral issues including gum diseases, cavities, and even whiten your teeth. If you have questions about which oral probiotics to use, contact our office today.
Wrapping up, oral health is important because it reflects your overall health. To achieve and maintain your best oral health, white smile and fresh breath, pay attention to your diet and daily habits, the frequency and consistency of brushing and flossing your teeth, and try out any of the extra tips mentioned in the article.
And last but certainly not least, if you have issues or doubts, you should get in touch with your dentist immediately. The post How to Easily Master Oral Health appeared first on Fort Worth Dentist | 7th Street District | H. Peter Ku, D.D.S. PA. via Blogger How to Easily Master Oral Health Cavity: a word no one wants to hear from their dentist. The story of cavities goes way back, with their age-old presence proven when a team of archaeologists discovered the teeth of our friend “John,” aged about 15,000 years old. And guess what? John’s teeth were riddled with holes because of cavities.
Cavities are also very widespread today. According to a 2016 study by the Centers for Disease Control and Prevention, more than 90% of U.S. adults have had a cavity and about 50% of all adults aged 30 or older have signs of gum disease. Cavities may form in the outer coating and the inner layer of a tooth, or in the gumline. Causes and complications of cavities--and gumline cavities, specifically
Cavities are caused by an entire ecosystem of bacteria living in our mouths. We actually have more bacteria in our mouth (20 to 100 billion) than the entire human population on Earth!
However, this number shouldn’t scare you, because most bacteria in our mouths are harmless. Bacteria in general feed on the foods and drinks you consume, and as living beings, they grow, move, reproduce and discharge waste matter. Depending on what we eat, and specifically how much sugar we consume, certain bacteria can overpopulate and cause the waste matter that causes cavities.
Jus like us humans, bacteria love sugar. They use it as an energy source, and when they consume it they release byproducts in the form of acids. These acids then stick to and start dissolving the minerals that make up tooth enamel, which is the protective layer of our teeth. Over time, a pit develops in the tooth and a cavity is formed.
Plaque can then build up in those pits as well as in the spaces between your teeth and along the gumline. If left unchecked, it may result in a gumline cavity.
Cavities can have serious and long-lasting complications for anyone, even to children that have not developed their permanent teeth yet. Some of these complications include:
Who is at higher risk? And how do you prevent gumline cavities?
Gumline cavities and cavities in general can occur to any age, and no matter the number of teeth. Culotta-Norton, former president of the D.C. Dental Society, told Live Science that some groups do have a higher risk for cavities, however, due largely to access to oral care and other factors. These groups include:
The key to prevent cavities is good dental and oral health. The following tips will help you maintain a healthy mouth, and will highly reduce the chances of getting a cavity or a gumline cavity.
Brush, brush, brush!
This is the most obvious tip and we are sure you’ve been hearing it since you were a child. However, now that you know about the billions of little bacteria that inhabit your mouth, we’re hoping you won’t take it lightly!
Brushing your teeth properly can keep your teeth and mouth healthy and strong. Always brush your teeth, taking care to brush down to the gumline, twice a day for two minutes with a soft toothbrush. And don’t forget to replace your toothbrush at least every 3 to 4 months. Finally, clean between your teeth once per day with dental floss to remove plaque that’s hard to reach with a toothbrush.
Also be sure to use a fluoride-containing toothpaste, because according to the American Dental Association, when the fluoride compounds are present in your mouth they can actually make your teeth stronger and prevent cavities. They can even reverse early tooth decay.
Fluoridated water, in particular, can do miracles in preventing cavities for the whole community. Studies have shown that that water fluoridation can reduce the amount of decay in children’s teeth by 18-40%.
Diet and smoking
Remember our friend John from before? John’s cavities were formed 15,000 years ago by the same thing that form our cavities today: bacteria. And although John’s diet did not contain processed sugars, the carbs from his rich in nuts–and–vegetables diet were broken down into simple sugars that bacteria could still feed on.
To avoid cavities, you must stop feeding those “naughty” bacteria that live in your mouth with processed sugar. Consume nutritious foods and try to avoid foods and snacks high in sugars as well as sweetened beverages such as sodas and energy drinks. If you have to consume a food high in sugar, brush your teeth shortly after.
You’re probably aware of the negative effects smoking can cause to overall health, too. According to the College of Dentistry, “smoking can do a lot more than just stain your teeth--this unhealthy habit can also lead to gum disease, tooth loss, and even oral cancer.” Try to quit smoking for both your overall and your oral health.
Visit your dentist regularly
Regular dental checkups are another key factor to reduce your chances of getting a cavity or gumline cavity. Your dentist will provide you with professional hygienic cleaning procedures that remove plaque and keep your teeth and gumline secure from cavity risk. In addition, the dentist will examine your mouth and spot other potential risks as well as the early signs of tooth decay.
Treatment for cavities
The idea of having an electric drill in your mouth doesn’t sound terribly appealing to anyone. But let’s get back to our friend John for a second. Archeological findings have shown that about 14,000 years ago, sharpened stone tools were used to remove bits of rotten teeth and cure cavities for John and his friend! We choose to feel thankful to have the tools available today—any drill will trump stone tools to fix tooth decay.
Filling a tooth with materials such as dental amalgam or composite resin is the most standard treatment for cavities in our day and age. Your dentist starts by removing the decayed material with a drill or laser, and then fills the hole in. Cavities along the gumline are treated in the same way. However, based on the severity of the damage to both the tooth and gumline, your dentist may choose another treatment plan, such as crowns or root canals.
Cavities are wide-spread and can cause a lot of complications, but they are also easily preventable. Cavities prevention starts by practicing good oral health from an early age, and decay can be later prevented with a proper diet and regular dentist visits. The post Gumline Cavities—How They Form And Tips To Prevent Them appeared first on Fort Worth Dentist | 7th Street District | H. Peter Ku, D.D.S. PA. via Blogger Gumline Cavities—How They Form And Tips To Prevent Them Sweet treats…a temptation for both children and parents (if we’re honest).
Would you be surprised if we started by reminding you that children love sweets?
Of course not! There’s even scientific evidence out there that shows children don’t just like sweets, they’re biologically hardwired to them.
Julie Mennella of the Monell Chemical Senses Center explains in recent research, “the newborn can detect sweet acutely, and will actually prefer sweeter solutions to less sweet ones. The basic biology of the child is that they don’t have to learn to like sweet or salt. It’s there from before birth.” Monella’s research also demonstrated that sugar helps children tolerate pain, and that it’s a natural pain reliever for them (wow)! On the other hand, sweet treats are also tempting for parents to use as rewards for their children’s good behavior. Although it’s seemingly the quickest and easiest way to reward your child and will definitely earn a few smiles, there’s a catch here. By using sweets as a reward, we risk building a bad habit for kids because we teach them that sweets can be better than others (by merit of the fact they’re seen as a “special reward”).
We come by our sugar fix naturally, but consuming too much can have shocking effects on your child’s oral and overall health. In this article, we’re going to talk about the dangers of sugar, yes, but (more importantly) the ways to simply cut down the sweets intake (and cravings) of your child.
First things first--how much sugar is OK?
The American Heart Association (AHA) recommends that children between 2 and 18 years old should all eat less than 25 grams--or six teaspoons--of added sugars daily. And yes, we are talking about refined sugar, not the natural sugar you find, say, in broccoli.
The AHA goes on, “Children and teens should limit their intake of sugar-sweetened drinks, specifically, to no more than eight ounces (or one glass) weekly.”
These recommendations also advise that children under the age of two should have no added sugars at all.
The same AHA publications also drops the handy reminder that the estimated volume of calories a child needs ranges from 1,000 a day for a sedentary two-year-old to 2,400 for active 14-18 years old girls and 3,200 for active 16-18 years old boys. Check the sugar content on foods and drinks, because it will have a direct impact on the number of calories consumed.
According to Miriam Vos, M.D., Ms.P.H, “if your child is eating the right amount of calories to achieve or maintain a healthy body weight, there isn’t much room in their food ‘budget’ for low-value junk foods, which is where most added sugars are found.”
Sweet treats and sugary drinks are rich in calories at the same time that they’re poor in nutrients. Most added sugars can be found in sodas, energy and food drinks, cookies and cakes, ice cream, candies, and other desserts. And no, those don’t form part of the food pyramid.
Consuming foods high in added sugars at a young age has also been linked to other risk factors such as increased risk of obesity, elevated blood pressure, diabetes, dyslipidemia and, of course, tooth decay.
How sugar affects oral health
You (and even your kids) already know that too much sugar will affect oral health. But let’s take a look at the “why.”
To begin with, sugar itself is not the issue, rather what happens after consuming it. Our mouths are full of bacteria, many of which are beneficial to our oral health. When we consume too much sugar, however, the “naughty” bacteria will use it as a fuel and break it up, thus producing acids. These acids will then stick and start dissolving the minerals that make the enamel, which is the protective layer of our teeth.
This “feeding” on the enamel will result in cavities and tooth decay.
How to (realistically) cut back on your child’s sweets consumption
With all those delicious temptations a breath away, and provided that children are biologically hardwired to love sweets, cutting back on candies can be a daunting task for many parents and caregivers. However, the health benefits will be long-lasting and definitely worth the effort.
We even have a list of tips to make the process easier. How’s that sound?
1: Make fruits the first choice to “satisfy sweet”
Fruits can be as delicious as sweets, especially after a short adjustment period where the palette “resets” to natural sugars (at which point fruit naturally tastes sweeter). Plus, fruits are packed with vitamins and nutrients essential for your child’s growth. As if you needed more reason, they also have fewer and healthier calories than foods with added sugar. And last but certainly not least, there is even a connection between a child’s low-quality diet (without fruits) and performance at school.
So, to make more fruit-eating happen:
2: Don’t offer sweets as rewards
As mentioned earlier, the easiest way to reward your children seems to be by offering them sweets. However, you build a bad diet as well as bad habits for children by doing this because you ultimately teach that sweets are more exciting than healthier foods. Consider rewarding your child with something like an activity, hugs and kind words. In addition, you can give your child other no-food rewards like stickers or drawing tools.
3: Drink responsibly!
Sugar-sweetened drinks such as soda contain a lot more sugar than you realize, and they are also high in calories and low-to-nothing in what they offer in nutrition. When your children are thirsty, give them water (and set the crucial example of drinking more of it yourself).
4: Keep sweets for special occasions
If we’re honest, it’s realistically OK for your child to eat candies on Halloween or other special days. Let your child enjoy them, and link candies and other sweets only to special occasions such as Halloween. You don’t have to worry about one day of the year, or even two or three, but you should be careful about the rest. If your child asks for some candy on non-special days, you can consider some, but only in small portions.
5: Be creative with snacks
Healthy foods may not look as fancy or enticing as candies and sweets. However, with just a bit of creativity, you can make your children love their new snacks! Bright colors and exotic textures can do the trick, both of which are abundant in the world of fruits and veggies.
And back to an earlier idea, you can also play games with healthy foods (gamification, we call it these days), such as encouraging your child to find the amount of total sugars on the Nutrition Facts label in foods to compare them with healthy foods they like. Or how about an apple tasting? Or letting your kids pick out the fruits in the grocery store for the fruit salad party at home?
Cutting down your children’s consumption of sweets might look like a tough task. However, the long-lasting health benefits are without a doubt worth the effort. So, arm yourself with patience and a little bit of creativity, and remember that it’s about progress today, not perfection! The post 5 Fun Tips to Tame Kids’ Temptation for Sweets appeared first on Fort Worth Dentist | 7th Street District | H. Peter Ku, D.D.S. PA. via Blogger 5 Fun Tips to Tame Kids’ Temptation for Sweets The American Dental Association posted a recent video that many won’t want to see, but must--the negative health issues (including fatal oral health complications) that smoking can produce.
The ADA’s video mixes vital facts with gripping visuals to amplify our understanding of the dangers of smoking in the only format many of us are impressed by anymore—video.
The effects of smoking on your oral health goes beyond yellowing of your smile; it causes serious complications, including the very real possibility of oral cancers.
Oral cancer can be aggressive and spread quickly due to the number of blood vessels in your head and neck along with the proximity to your lymph nodes. And while the use of tobacco has been on the decline in the last 20 years, approximately 15% of all Americans still smoke.
Smoking’s effect on the mouth
For many of us, the first thing we notice when someone smokes is the yellow tint to their teeth. The yellow “cooling” is caused by chemicals found in cigarettes that stain the enamel of the teeth. Enamel is one of the hardest substances in the body; however, once it is damaged or eroded, there is no bringing it back.
Infected and receding gums are another sign of a smoker. Smokers are twice as likely to suffer from gum disease as nonsmokers. When the gums are damaged, they can pull away from the teeth and cause the bones underneath to deteriorate. And once the bones break down, it causes instability in the teeth and can cause them to become loose and fall out. This is why many smokers are lacking at least one tooth.
Finally, smoker’s breath is another adverse effect of smoking that virtually all of us are familiar with. Particles from the cigarette are transferred to the mouth where they remain long after you put out the cigarette. These particles can dry out your mouth, which causes bacteria to multiply. The common lack of salvia among smokers spurs this bacteria to attach to the teeth and gum line, too, which is how periodontal diseases are caused.
The most severe complication that can occur due to smoking is oral cancer. It is estimated 80% of those diagnosed with oral cancer are also smokers. Early symptoms of include swelling or lumps around your mouth, red or white lesions in your mouth, and numbness and trouble moving your jaw when talking or eating. If you are experiencing any of these symptoms, it is important you seek medical care immediately.
Electronic cigarettes and smokeless tobacco
Even though you aren’t “smoking it,” smokeless tobacco can still cause significant oral health problems. Just like cigarette smokers, those who use smokeless tobacco are still plagued with bad breath, teeth discoloration and a greater risk of developing periodontal diseases. In fact, smokeless tobacco can increase the risk of periodontal disease even over the rates seen in cigarette smokers. Those who use smokeless tobacco need to visit their dentist more frequently, since oral lesions and other complications can develop quickly and become serious if left unchecked.
Electronic cigarettes are another popular option for people who want to still have the feeling of smoking but—supposedly—without the same concoction of chemicals, and sometimes without the nicotine. These devices have received quite a bit of attention as health professionals determine if they are harmful.
And while these products do have the potential to reduce tobacco use, it is important to remember that no product you inhale is guaranteed safe. Using e-cigarettes can still bring your mouth into contact with nicotine. This can reduce blood flow to the mouth and cause tissues to lose oxygen and nutrients. And when blood vessels contract, it can cause gum line recession and all the other symptoms of chronic cigarette smoking. E-cigarette use can also lead to dry mouth, which allows bad bacteria to multiply and result in cavities or other infections.
If you choose to use e-cigarettes to transition away from smoking, it is important you tell your dentist and continue to go to your regular appointments. Your dentist will be able to spot signs of periodontal disease.
Any time you are inhaling a product--tobacco laced or not--there is the potential for harm to the mouth as well as the throat and lungs. If you are a smoker, it’s important to let your dentist know what type of product you consume so they can screen you more frequently for cancer risks and oral health diseases. The post What You Don’t Want To Read, But Need To See, About Smoking And Your Mouth appeared first on Fort Worth Dentist | 7th Street District | H. Peter Ku, D.D.S. PA. via Blogger What You Don’t Want To Read, But Need To See, About Smoking And Your Mouth When we talk to some of our patients about the problems they face, whether it comes to dental care or oral health, we continually hear one issue: dental care is a financial burden.
Some of our patients with the most complex cases admit they realized they may need to wait seek care months or years prior to coming into our office. However, the fear of the bill or the inability to pay in the moment results in them delaying care—often to the detriment of their oral health. The longer care is delayed the more complex the oral health condition becomes. In addition, it can begin to interfere with other bodily systems such as an increased risk of heart disease or complicate diabetes. If you are living in Fort Worth and in need of dental care, but unsure about how to pay, then give our office a call today. In addition, we have outlined ideas below on how to plan and afford dental services.
Enroll in dental insurance
Monthly dental insurance can be an affordable option if you find the plan that works for you. Depending on the benefit structure, some plans can be as low as $25 a month.
While each dental insurance benefit is different, many times preventive care (such as your bi-annual cleaning) will have a very low out-of-pocket cost for the beneficiary. In effect, you’re paying for service with the premiums that will be reimbursed to the dentist by your insurer.
And in addition to generally-covered preventative care, many plans also have annual out-of-pocket limits. If you or your family has had significant dental care costs this year, you might be close to your annual limit. But this doesn’t mean you will be denied services! Instead, you have hit the maximum out–of–pocket you have to pay, and the insurer will now pick up the remainder of needed services. These maximums normally run year to year, so by slipping into the next year will mean the number resets. Take advantage of these plans before the end of each year to stay ahead of bigger dental issues later.
Flexible spending accounts
Flexible spending accounts are a great way to save pre-tax dollars to be used for certain qualified medical and dental expenses. After signing up for an FSA, the money is automatically deposited in an account that you can draw on when you receive a medical or dental bill.
And due to the tax savings, you come out ahead financially. However, unlike a health savings account (HSA) that can be rolled over year to year, an FSA must be spent by the end of the year. If you forget to spend the money, there is no getting it back.
Ask for new patient specials
If you’ve avoided dental care for years due to the cost, then you are probably in the market for a new dentist. Many dentists run new-patient specials that target issues such as missing teeth, deep cleaning services and consultations on other more complex services you might need. Even if it isn’t listed on a dentist’s website, give them a call and ask if they offer any benefits for new patients.
And once you find a dentist you like, ask about referral programs, too!
Discuss payment plans
We understand that complex dental care can be expensive. Therefore, we work with you on options like payment plans to allow you to get work done while paying it back on a schedule that fits your needs. We want to remind our patients that there is nothing shameful about asking for a payment plan. In fact, we would prefer that we have that conversation instead of having to discuss complex care plans that could have been prevented if you would have sought care earlier.
Our goal is ensure that all our patients get quality and affordable dental care. Your health is of the upmost importance to us. Please always feel that you can bring up any issue--including financial issues--with us, so give us a call today! The post What Are The Best Ways To Pay For Dental Costs? appeared first on Fort Worth Dentist | 7th Street District | H. Peter Ku, D.D.S. PA. via Blogger What Are The Best Ways To Pay For Dental Costs? The mouth is commonly described as the “window to the body” and your overall health. Did you know that the teeth and gums are sometimes the first indicator that there is a medical problem in another system?
It’s important to remember that your mouth is not a separate entity separate from the rest of your body, rather an intricately intertwined consideration for your total body health. In addition to the mouth highlighting issues with other body systems, problems in your mouth can even cause problems elsewhere in your body. Think of the relationship between total body health and oral health as a two–way street. They both affect the other. Keep reading as we discuss how our oral health is connected to all aspects of our health.
The connection between mental and oral health
Thanks to mental health awareness and greater transparency and open discussions on the topic, there’s been more research about the connection between oral and mental health in recent years.
The most common mental health conditions that affect oral health are anxiety and panic attacks, depression, eating disorders, obsessive-compulsive disorder, self-harm, schizophrenia and psychosis. The varying severity of these mental illnesses can cause neglect of oral health routines which can lead to tooth decay, gum disease and tooth loss. To read more about the interaction between mental and oral health, read What DentalHealth.org has to say on the topic.
Oral health and small children
You’ve probably heard about babies catching colds or more serious communicable diseases from adults, but what about catching cavities? That seems almost preposterous! However, researcher has shown that adults who transfer salvia to their baby may be also passing cavity causing bacteria. This can occur through kissing, sharing utensils or sharing bites of food. These germs can start the process that causes cavities even before babies have teeth, so it’s important to avoid sharing saliva with your baby right from the start.
Dry mouth
Side effects of medication are the primary cause of dry mouth. Medications such as and anti- histamines and decongestants--both which are commonly used during North Texas allergy season--can cause a decrease in salvia production.
Lack of salvia and severe dry mouth can lead to serious oral and health complications. First, increased plaque, tooth decay and gum disease can occur in patients. Saliva neutralizes bacteria by limiting bacterial growth and washing away food particles. Other complications include mouth sores, yeast infections in the mouth and split, dry skin around the mouth and lips. Finally, saliva enhances a person’s ability to taste, swallow and digest food.
Many of our older patients complain about dulled tastes, which can be tied back to dry mouth. If a decrease in salvia results in difficult chewing and swallowing, a patient’s nutrition could be affected, causing even more problems.
Immune system
If you are experiencing severe dry mouth (and aren’t on any medications that can cause this side effect) then you might be suffering from an autoimmune disease. Most doctors and dentists commonly associate dry mouth with Sjogren’s syndrome, which is caused by the body attacking the glands that make saliva and tears. Prolonged dry mouth can lead to an increased risk of cavities. In addition, Sjogren’s syndrome commonly accompanies other autoimmune diseases such as rheumatoid arthritis and lupus. If you are experiencing extreme dry mouth, it’s important you make an appointment with your dentist or doctor.
Is there a connection between heart and oral health?
Studies have shown that there is a link between gum disease and heart attacks or strokes. It’s thought that, since gum disease is bacteria-caused, it can enter your bloodstream where the bacteria attach to the fatty deposits in the heart blood vessels. This condition can cause blood clots and may lead to heart attacks. In the absence of gum disease, scientists have found there is less bacteria in the heart.
Diabetes and oral health
Periodontal disease is caused by bacteria in the mouth that infect the gum tissue and cause plaque. Poorly managed blood sugar--common in those not yet diagnosed with diabetes--causes damage to blood vessels, which leads to oxygen restriction and nutrition deprivation to the gums and bones. Higher glucose levels in salvia create a breeding ground for bacteria. Weak gums and bone will be targeted by the bacteria and result in oral health diseases.
Concerned about your overall health? The first stop might be the dentist! Give us a call today. The post How Oral Health Equals Whole Body Health appeared first on Fort Worth Dentist | 7th Street District | H. Peter Ku, D.D.S. PA. via Blogger How Oral Health Equals Whole Body Health There are many milestones that mark a coming of age. At 16 you can get your driver’s license, at 18 you’re a legally an adult and most kids then graduate high school and head off to college.
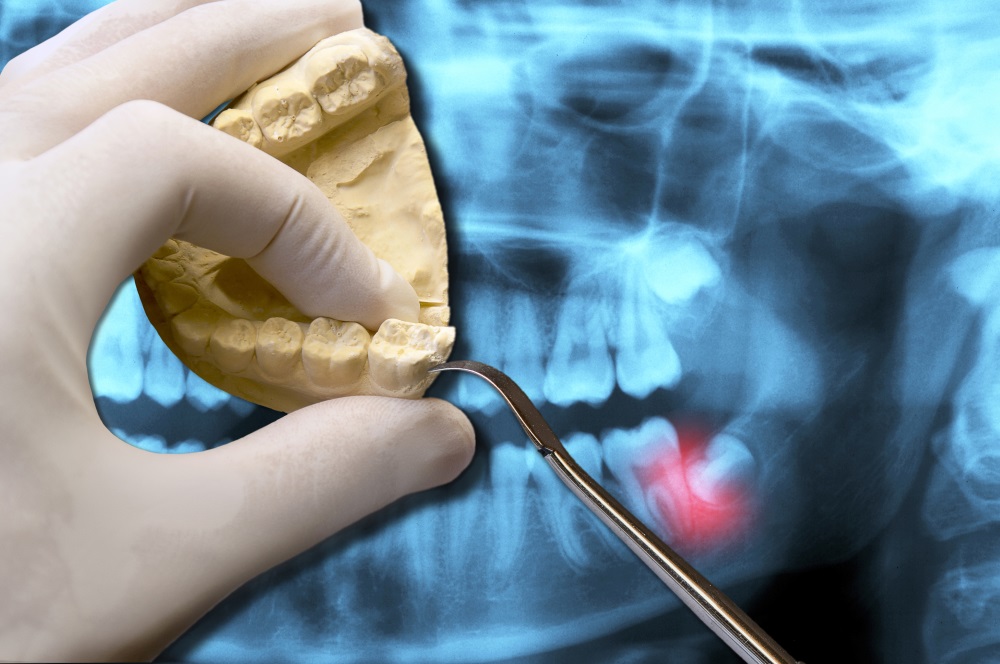
Just like these milestones, there are also several key dental milestones. Your parents remember your first tooth erupting (and the many more that came after), the first tooth you lost, any orthodontic work you had done, and finally getting your wisdom teeth removed. For the younger generations, most of us remember getting our wisdom teeth out over summer break or between semesters in college. However, removing wisdom teeth hasn’t always been standard. In fact, one common question we get from our older patients who still have their wisdom teeth is if we still need to remove them. Just like with your appendix, wisdom teeth are fine to have until something goes wrong or a risk is identified. And when that happens, it normally requires immediate action.
If you still have your wisdom teeth, it’s important to discuss them with your dentist and determine if they could be doing more harm than good.
Why do we have wisdom teeth?
Sometimes more accurately referred to as our third set of molars, wisdom teeth were necessary once upon a time when our ancestors subsisted on a diet that consisted of tough meats and fibrous roots. In addition, these ancestors had much larger mouths, which could easily fit 32 teeth.
However, as humans evolved and we left the hunter and gatherer lifestyle, our jaws also changed. Thanks to softer foods and more diverse diets, we no longer needed an extra set of molars to help break down food. And with a smaller jaw, 32 teeth could no longer fit properly. Due to this, complications have become common, like teeth that don’t fully erupt and become impacted. Pain and infection always follow.
How did wisdom teeth get their name?
Third molars have been referred to as “teeth of wisdom” since the 17th century and just as “wisdom teeth” since the 19th century. These third molars generally appear much later than other teeth, usually between the ages of 17 and 25 when a person reaches adulthood. It’s generally thought today that they’re called wisdom teeth because they appear so late, at an age when a person matures into adulthood and is “wiser” than when other teeth have erupted. We won’t comment on the “wise” nature of 17 to 25-year-olds, but we’ll agree that these late-erupters definitely come at a later stage of life.
I’m an adult and still have my wisdom teeth, now what?
Dentists and oral surgeons don’t recommend removal just so we have something to do! Instead, we see the problem with wisdom teeth when there is no longer room for them in the mouth, resulting in poor root quality and oddly-shaped or angled teeth. Even if you do have the space in your mouth, there is a higher likelihood that your wisdom teeth could become infected or lead to the development of other periodontal diseases since they’re so far back in the mouth and that much harder to clean. Many times, pulling wisdom teeth is a preventative measure that is done to protect the long-term health of your mouth.
While there is no “correct” time for wisdom tooth removal, the younger you have it done, the easier the healing process. The procedure to remove wisdom teeth varies from patient to patient since sometimes the teeth are impacted or a patient may not have a full set. The procedure shouldn’t be painful with the correct anesthesia, and is almost always done in an outpatient setting. Proper care after the procedure is important to prevent painful side effects like dry sockets.
Removal prior to wisdom teeth causing a problem or resulting in more significant dental work is important. If you or your child still have wisdom teeth and you are looking for a consultation, give our office in Fort Worth a call today! The post The History of Wisdom Teeth appeared first on Fort Worth Dentist | 7th Street District | H. Peter Ku, D.D.S. PA. via Blogger The History of Wisdom Teeth |
Who We Are
If you reside in Fort Worth and never visited dentist, you should note that your first dentist visit generally includes a Comprehensive Dental Examination. We will diagnose your unique dental needs, learn your desires, and discuss how we might fulfill them.
Social Links
Dentist Fort Worth
Dentist Fort Worth Diigo Dentist Fort Worth Disqus Dentist Fort Worth Tumblr Dentist Fort Worth Twitter Dentist Fort Worth G Drive Dentist Fort Worth Medium Dentist Fort Worth Onenote Dentist Fort Worth Gravatar Dentist Fort Worth Alternion Dentist Fort Worth Blogger Dentist Fort Worth Evernote Dentist Fort Worth Pinterest Dentist Fort Worth Facebook Dentist Fort Worth Getpocket |





 RSS Feed
RSS Feed
